The U.S. Department of Justice recovered $1.67 billion in healthcare-related False Claims Act (FCA) settlements in fiscal year 2024. Many of these enforcement actions trace back to a familiar compliance gap: contracts that fell out of alignment with current regulations and went unreviewed.
This is a pattern across healthcare organizations. A vendor's Business Associate Agreement (BAA) auto-renews, carrying forward outdated HIPAA clauses that no longer meet federal requirements. A payer contract keeps running on terms that predate the latest state health data amendments.
Both contracts are technically active, both create real compliance exposure, and both went unflagged because no structured review process existed to catch them.
Every vendor accessing Protected Health Information (PHI) must operate under a current, HIPAA-compliant BAA that makes privacy and security obligations contractually enforceable. When those agreements retain legacy language or miss required regulatory updates, the organization faces financial penalties, legal exposure, and audit findings.
A healthcare contract compliance audit helps catch these gaps before they escalate.
In this guide, you will learn:
- What a contract compliance audit is and why it matters in healthcare
- The most common risks and red flags that audits reveal
- Steps to perform a healthcare contract compliance audit
- A practical checklist to keep your organization audit-ready
- How to utilize Signeasy to streamline the process
What is a contract compliance audit in healthcare?
A contract compliance audit in healthcare is a structured review of your organization's agreements with vendors, payers, physicians, and partners. It evaluates whether each contract's terms are current, legally enforceable, and aligned with the latest federal and state regulatory requirements.
In healthcare, the scope of this audit extends across multiple contract types: payer contracts, physician employment contracts, vendor and supplier deals, Business Associate Agreements (BAAs), and managed care arrangements.
Healthcare contracts carry a level of risk that most commercial agreements do not. They govern access to PHI, determine reimbursement terms worth millions of dollars, and must satisfy strict regulatory frameworks like HIPAA, Stark Law, and the Anti-Kickback Statute.
When obligations in these contracts are missed or outdated, the consequences are specific and serious. Overpayments go undetected, HIPAA violations trigger six-figure penalties, payer disputes escalate into audits and clawbacks, and physician compensation arrangements fall out of fair market value compliance.
General compliance audit vs. healthcare compliance audit
A general compliance audit evaluates the larger company and a healthcare compliance audit narrows on maintaining compliance in healthcare. Here’s how the two differ:
Why healthcare organizations need contract compliance audits
Healthcare organizations manage PHI and Personally Identifiable Information (PII) across every vendor, payer, and partner agreement. These contracts are typically fragmented across legal, compliance, revenue cycle, IT, and procurement, making gaps easy to miss.
Each gap can independently trigger an OCR investigation, a payer recoupment, or a False Claims Act inquiry.
Here are the areas where contract compliance audits deliver the most value:
- Billing inaccuracies and overpayments: Healthcare billing depends on payer-specific reimbursement logic, negotiated fee schedules, and precise contract terms. When any of these fall out of date or get misapplied, organizations face overpayments, underbillings, and revenue leakage that often goes undetected until a payer audit.
- Expired or auto-renewed contracts: When renewal dates and termination windows are not actively tracked, agreements roll over automatically. This means expired terms, outdated pricing, and non-compliant clauses silently carry forward into active contracts, creating compliance exposure that no one is monitoring.
- Missing or incomplete BAAs: Every vendor, partner, or subcontractor with access to PHI is required to operate under a current, HIPAA-compliant BAA. Without one, the organization has direct regulatory exposure from day one.
- Undocumented amendments: Changes to payment terms, service scope, or delivery timelines often happen informally, through emails, verbal agreements, or side conversations. Without formal documentation, these changes become invisible and can trigger reimbursement disputes, payer audits, and regulatory enforcement actions.
- Vague compliance clauses: Generic regulatory language may have passed review at the time of signing, but falls short when HIPAA or Stark Law requirements change or enforcement tightens.
- Unclear audit trails: If your organization cannot show who approved a contract change, when it happened, and what was modified, it weakens your position in any regulatory review. Missing or undocumented contracts can directly affect patient safety, care continuity, and the protection of sensitive health data.

What are the types of contract compliance audits in healthcare?
The type of audit depends on what your organization needs to evaluate, whether that is regulatory adherence, financial accuracy, vendor performance, or internal policy alignment. A strong healthcare contract management strategy includes a mix of these audit types based on risk priority and organizational needs:
- Regulatory compliance audit: Reviews contracts for alignment with HIPAA, Stark Law, Anti-Kickback Statute (AKS), and state health data regulations.
- Financial compliance audit: Evaluates billing terms, fee schedules, reimbursement accuracy, and payment obligations against payer contracts.
- Vendor and BAA audit: Confirms that all third parties accessing PHI have current, enforceable Business Associate Agreements in place.
- Physician and referral arrangement audit: Assesses physician compensation agreements for fair market value compliance and referral integrity under Stark Law and AKS.
- Operational compliance audit: Checks whether service delivery, performance benchmarks, and SLAs outlined in contracts are being met.
- Internal policy audit: Verifies that contract management practices align with the organization's own compliance policies, approval workflows, and documentation standards.
Suggested read: 15 Healthcare Contract Management Best Practices
How to perform a healthcare contract compliance audit (Step-by-step)
Step 1: Define the audit scope and objectives
Start by identifying which contract category you are auditing (vendor agreements, payer contracts, BAAs, or physician arrangements), what triggered the audit (a regulatory update, a renewal cycle, a billing discrepancy, or an internal compliance concern), and what the audit needs to answer.
For example, the objective might be to confirm that all vendor BAAs reflect the latest HIPAA Privacy and Security Rule requirements, or to verify that payer reimbursement terms match what is actually being billed.
A clear scope ensures the right stakeholders from legal, compliance, revenue cycle, or procurement are involved and that the audit surfaces actionable findings.
Step 2: Assemble the audit team and assign roles
Depending on the audit scope, assemble a team that reflects the contracts being reviewed. A BAA audit requires legal and IT security, a payer contract review needs revenue cycle and finance, and physician arrangement audits call for compliance and clinical operations.
Assign specific roles and responsibilities:
- One person should lead the audit and coordinate timelines.
- Others should be responsible for gathering contracts, reviewing specific sections, or verifying financial terms.
- For audits involving vendor contracts with PHI access, include someone with HIPAA knowledge who can evaluate data handling clauses and BAA completeness.
Step 3: Gather all relevant contracts and documentation
Pull together every contract, amendment, addendum, side letter, and supporting document within the audit scope. For contract compliance audits in healthcare, that includes:
- Original signed agreements
- Executed BAAs and any updates to them
- HIPAA-related amendments
- Payer fee schedules and reimbursement terms
- Physician compensation arrangements
- Vendor certifications and insurance records
- Correspondence that references or modifies contract terms
Gaps in documentation are often where compliance findings originate, so completeness at this stage is critical.
Step 4: Review contract terms against actual performance
With all contracts in hand, the audit team reviews each agreement line by line against what is happening in practice. This is the core of the audit:
- Payer contracts: Compare contracted reimbursement rates against actual claims data to identify underpayments, overpayments, or fee schedule mismatches.
- BAAs: Confirm that data handling, breach notification timelines, PHI access controls, and subcontractor provisions meet current HIPAA Privacy and Security Rule requirements.
- Physician arrangements: Verify that compensation structures remain within fair market value and comply with Stark Law and AKS thresholds.
- Vendor contracts: Check whether services delivered match the contracted scope and whether required compliance certifications and insurance coverage are still current.
Flag every gap, discrepancy, or area of concern for further review.
Step 5: Identify non-compliance and flag risks
Once the review is complete, consolidate all identified gaps into a single findings log and categorize each finding by severity.
High-risk items require immediate attention. Examples include:
- A vendor is handling PHI without a signed BAA in place.
- A physician compensation arrangement exceeds fair market value thresholds under Stark Law.
- A BAA still references pre-2013 HIPAA language and was never updated to reflect the Omnibus Rule.
- Billed rates on a payer contract do not match the contracted fee schedule, creating overpayment liability.
Lower-risk findings can be addressed in a standard timeline. Examples include:
- A BAA is fully compliant but missing a signature date.
- A contract references an outdated internal policy number but contains the correct obligations.
- An amendment was executed correctly but filed separately from the original agreement.
For each finding, document what the contract requires, what is actually happening, the specific gap, and the potential impact on compliance, finances, or operations.
Pay close attention to patterns. If multiple vendor contracts are missing the same HIPAA clause, the issue is likely in your contract template or review process rather than an isolated oversight.
Step 6: Communicate with third parties
Some audit findings will require action from the other party to the contract.
A vendor may need to sign an updated BAA that reflects current HIPAA Privacy and Security Rule requirements. A payer contract may need renegotiation to align reimbursement terms with updated CPT or billing codes. A physician group may need to revise a compensation arrangement to meet Stark Law fair market value thresholds.
Reach out to each third party with clear documentation of the gap, a specific request for resolution, and a reasonable deadline. Keep a record of all communications. Documentation here matters because it demonstrates good faith compliance efforts during any future OCR investigation or payer audit.
If a vendor or partner is unresponsive or refuses to address a compliance issue, escalate through legal or procurement. For BAA-related gaps, consider whether continued data sharing is appropriate until the issue is resolved.

Step 7: Build a corrective action plan
For every finding, assign a corrective action with a clear owner, deadline, and expected outcome. High-risk findings should have shorter timelines and senior-level ownership. Examples of corrective actions include:
- Updating BAA templates to include current breach notification timelines, subcontractor provisions, and PHI access controls
- Renegotiating payer contracts where billed rates no longer match the contracted fee schedule
- Executing new BAAs with vendors or subcontractors who are accessing PHI without a compliant agreement in place
- Revising physician compensation arrangements that fall outside fair market value under Stark Law
- Strengthening internal approval workflows to prevent undocumented amendments to reimbursement terms or service scope
Group corrective actions by priority and track them in a shared log that the audit team, compliance leadership, and legal can access.
Step 8: Document findings and schedule follow-ups
Compile all findings, corrective actions, and supporting evidence into a formal audit report. This report serves as your organization's compliance record and becomes critical documentation if an OCR review, payer audit, or False Claims Act inquiry occurs.
Share the report with relevant stakeholders, including compliance leadership, legal, finance, and department heads responsible for contract oversight. Schedule a review meeting to discuss findings and align on priorities.
Finally, set a date for the follow-up audit. A follow-up verifies that corrective actions were completed, confirms that fixes are holding, and catches any new issues that may have surfaced since the last review.
Suggested read: Contract Compliance Reporting: A Practical Guide
Healthcare contract compliance audit checklist
Use this checklist to stay organized before, during, and after every healthcare contract compliance audit cycle.
Pre-audit preparation
Contract review
Risk and compliance
Post-audit
How Signeasy simplifies healthcare contract compliance audits
Signeasy is a healthcare contract management platform that supports the compliance infrastructure that organizations need across every stage of the contract lifecycle. From signing and storage to tracking and retrieval, here’s how Signeasy helps you stay audit-ready:
1. Stay HIPAA-compliant with every signature
Every document signed through Signeasy generates a detailed audit trail that logs signer identity, timestamps, IP addresses, and device details. Healthcare organizations handling PHI can rely on these records as evidence during regulatory reviews.
A signed BAA is available for qualifying plans, supporting HIPAA-compliant eSignature use in accordance with regulatory requirements.
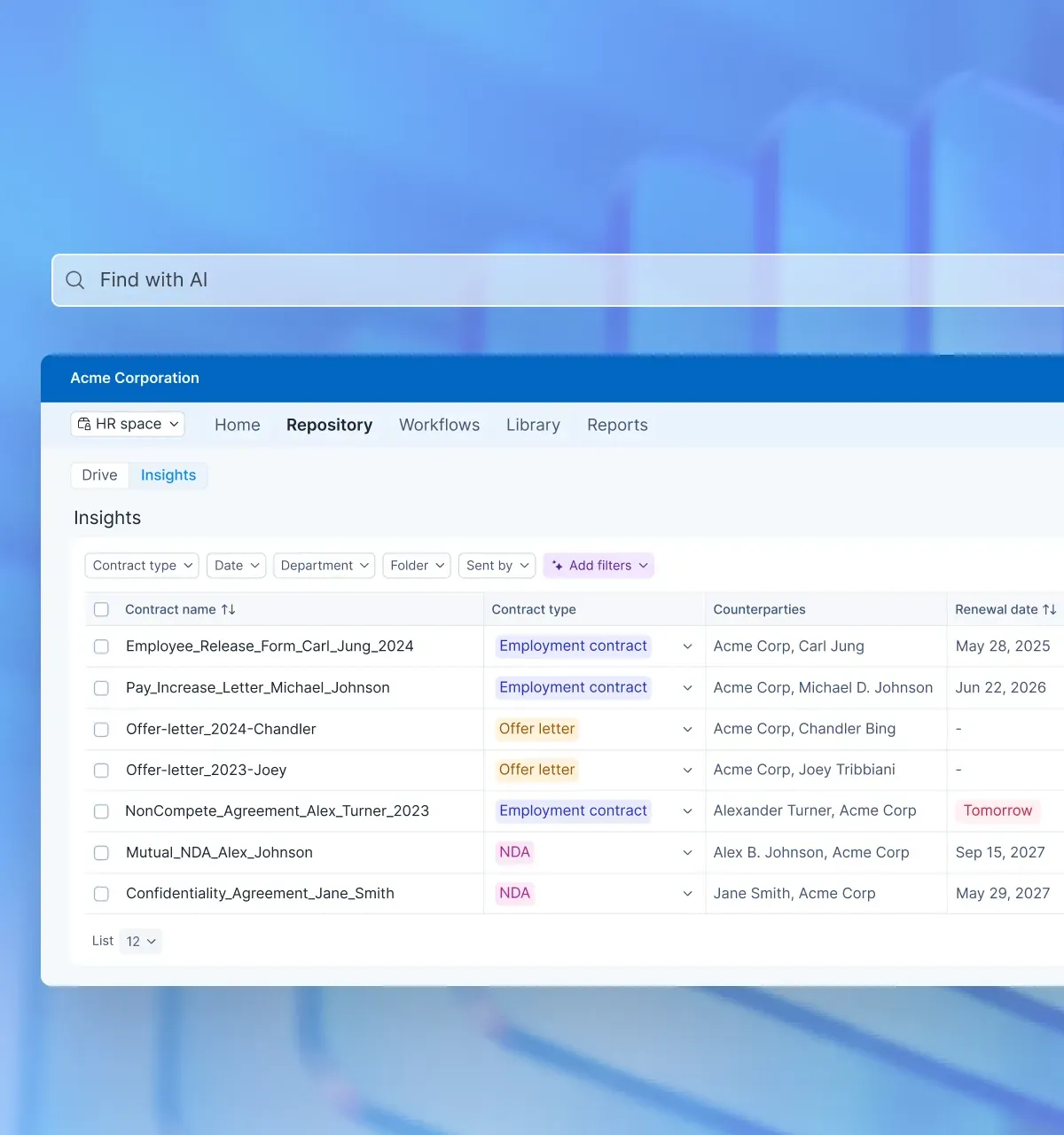
2. Centralize every healthcare agreement
Signeasy's Intelligent Contract Management stores every agreement in one secure location with status filtering (Needs Action, Waiting, Completed) and advanced search.
Instead of BAAs sitting with legal, payer contracts buried in revenue cycle inboxes, and vendor agreements scattered across procurement folders, every healthcare contract lives in a single, organized system.
Compliance teams can search by contract type, counterparty, status, or expiration date to instantly locate any BAA, payer agreement, physician arrangement, or vendor contract. Pre-audit contract gathering can now happen in minutes.
3. Keep contract deadlines on track with automated reminders
Contracts with pending signatures or approaching deadlines need consistent follow-up. Signeasy for healthcare sends automated reminders to signers and contract owners, keeping contract workflows moving without manual intervention.
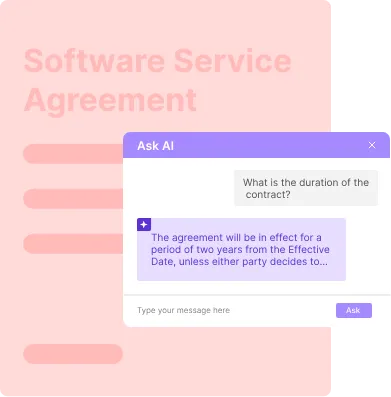
4. Review contracts quickly with AI-powered insights
Signeasy AI helps teams review contracts by generating summaries, extracting key terms, and answering natural language questions directly from the document.
During a healthcare enforcement review, compliance officers may need to confirm whether a BAA specifies HIPAA breach reporting within required timeframes, whether a managed care agreement permits retrospective claims audits, whether value-based compensation structures comply with Stark exceptions, or whether subcontractors are contractually bound to safeguard PHI.
You can get answers pulled straight from the agreement, rather than reading through every page manually.
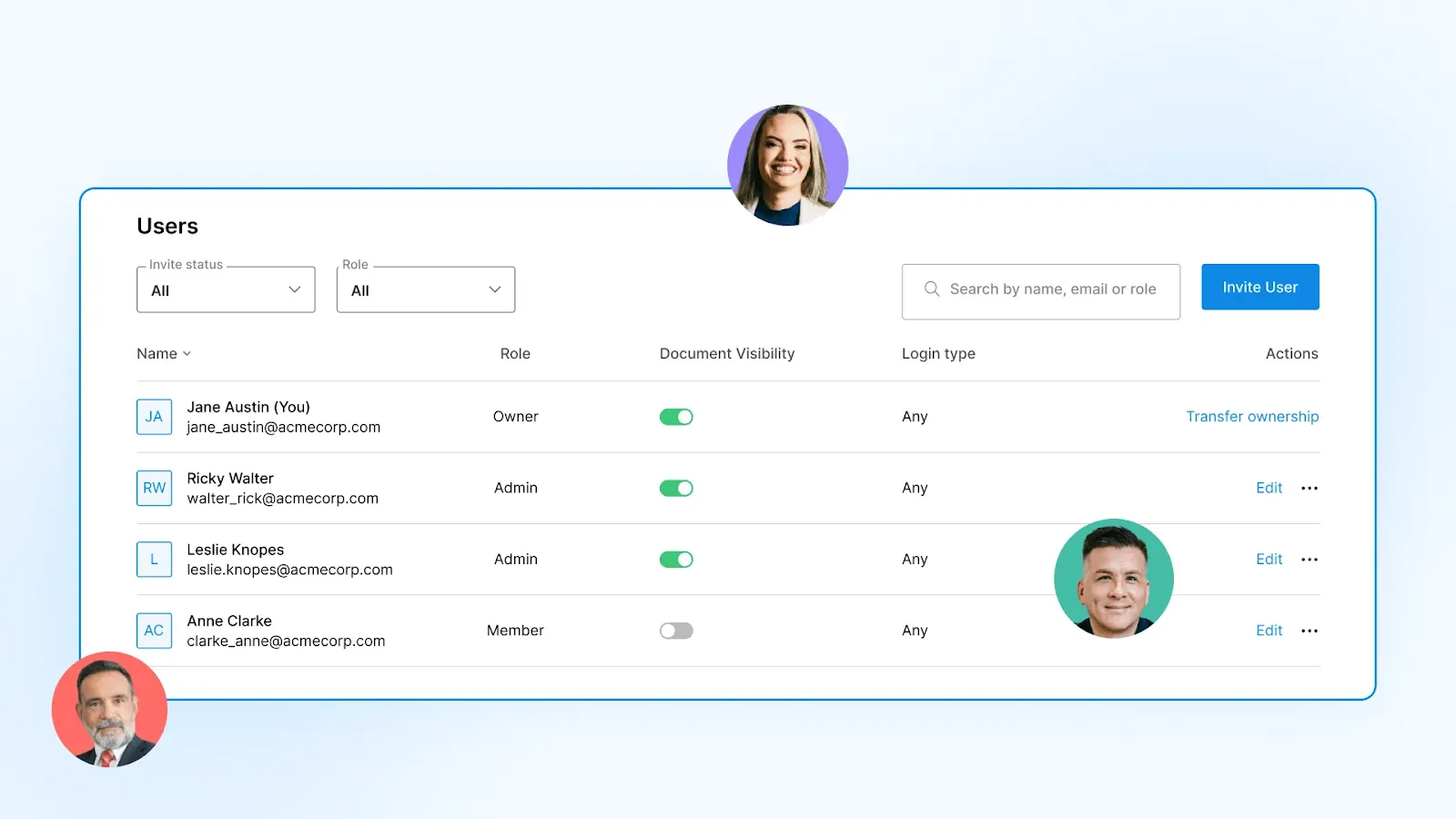
5. Control access with role-based permissions and 2FA
Administrators can assign permissions based on roles, ensuring that sensitive contracts are only accessible to authorized team members. Two-factor authentication (2FA) adds an extra layer of security for signers.
Together, these controls strengthen your organization's access management during audits and regulatory reviews.
6. Meet FDA requirements with 21 CFR Part 11 compliance
For healthcare organizations operating in FDA-regulated environments, Signeasy's Enterprise plan supports 21 CFR Part 11 requirements. It covers electronic signatures and electronic records in life sciences, clinical trials, and pharmaceutical workflows, ensuring that regulated documents meet federal standards.

Build a healthcare compliance-ready contract process
Every healthcare contract compliance audit comes down to one question: can your organization prove that its agreements are current, complete, and compliant?
The steps and checklist give your team a structured way to answer that with confidence, whether you’re preparing for an internal review or responding to external regulatory scrutiny.
Signeasy supports the entire healthcare compliance audit process.
A centralized, searchable repository keeps every agreement accessible, while automated reminders ensure renewals and critical deadlines stay visible. HIPAA-compliant contract workflows generate tamper-proof audit trails, and AI-powered insights reduce the time teams spend reviewing agreements during audits.
Start a free trial and simplify your next healthcare contract compliance audit.












.png)