The U.S. Department of Justice recovered $1.67 billion in healthcare-related False Claims Act (FCA) settlements in fiscal year 2024. A significant share of those cases traced back to documentation failures, missed obligations, and agreements that did not reflect current regulatory requirements.
It is easy to see how that happens. A typical healthcare organization manages hundreds of active agreements at a time. Each one carries regulatory obligations tied to HIPAA, Stark Law, or the False Claims Act. When those contracts live in spreadsheets, shared folders, or scattered email threads, deadlines slip, language goes unchecked, and audit trails disappear.
Contract compliance management in healthcare is the discipline of preventing exactly that. It involves monitoring, enforcing, and documenting adherence to every regulatory and operational obligation embedded in your agreements.
In this guide, you will learn:
- What does contract compliance management mean in healthcare
- Key regulations shaping healthcare contracts
- Practical tips for managing compliance across departments
- Ways automation and AI reduce manual effort and risk
- How Signeasy supports HIPAA-compliant contract workflows
What is contract compliance management in healthcare?
Contract compliance management in healthcare is the ongoing process of making sure every agreement your organization enters into meets its regulatory, financial, and operational obligations from execution through expiration.
But what makes healthcare contract compliance so different from standard contract management? It comes down to the regulations you're bound by, the risks of falling short, and the tools you need to stay ahead of both.
1. Healthcare contract compliance vs. general contract compliance
Most industries deal with contract compliance at some level, but healthcare adds layers of complexity that make it a fundamentally different challenge. The table below breaks down key distinctions, like data sensitivity, audit exposure, and penalty severity.
2. Types of contracts involved
Healthcare organizations manage a broad range of contracts, and each carries its own regulatory and operational obligations. These include:
- Payer agreements define reimbursement terms, billing codes, and timely filing requirements. Non-compliance often results in claim denials, underpayments, and revenue leakage.
- Physician and provider contracts must align with Stark Law and Anti-Kickback Statute provisions to prevent allegations of improper referral arrangements or inflated compensation.
- Vendor and supplier agreements cover medical devices, IT systems, and facility services. Many include data access provisions that trigger HIPAA obligations.
- Business Associate Agreements (BAAs) are legally required whenever a third party handles PHI on the organization's behalf. A missing or improperly drafted BAA remains one of the most common HIPAA violations.
- Managed care contracts govern network participation, credentialing, and quality reporting. Performance terms directly influence reimbursement rates and patient access.
Organizations that follow strong healthcare contract management best practices build compliance tracking into every contract type from the start. But no matter the contract type, the compliance requirements ultimately trace back to the same set of regulations.
Here's a closer look at the laws that shape how each of these agreements must be drafted, managed, and enforced.
Key regulations that affect healthcare contract compliance
Healthcare contracts do not operate under a single law. A single vendor agreement, for example, might need to account for patient data protections under HIPAA, referral restrictions under the Stark Law, and billing accuracy requirements under the False Claims Act — all at once. Below are the regulations that most directly shape how healthcare contracts must be structured and managed.
- HIPAA and HITECH govern the protection of PHI and require specific safeguards in any contract involving patient data, particularly BAAs.
- Stark Law and Anti-Kickback Statute (AKS) restrict financial relationships and referral arrangements between healthcare entities, making physician contracts and vendor agreements common enforcement targets.
- False Claims Act (FCA) holds organizations liable for submitting false or fraudulent claims to Medicare or Medicaid, putting billing and reimbursement terms under direct regulatory scrutiny.
- 42 CFR Part 2 imposes stricter-than-HIPAA protections for substance use disorder patient records, requiring heightened consent and disclosure standards in related contracts.
- 21 CFR Part 11 sets the FDA's standard for electronic records and signatures in regulated environments, affecting contracts tied to clinical trials, pharmaceuticals, or medical devices.
- State privacy laws in California, Texas, and New York enforce additional patient data, breach notification, and consent requirements that must be reflected in multi-state contract terms.
Even with these regulations well understood, compliance gaps still emerge when contract workflows can't keep up.
Suggested read: Contract management in healthcare: A comprehensive guide
What are the common contract compliance risks in healthcare?
Contract compliance risks in healthcare build up quietly through manual processes, scattered documents, and teams operating without shared visibility into contract obligations.
These are the risks that surface most often:
- Missed renewal and termination deadlines lock organizations into unfavorable terms or cause service lapses that disrupt patient care and vendor relationships.
- Inconsistent contract language across departments leaves agreements with outdated HIPAA or Stark Law clauses, creating regulatory exposure that only surfaces during an audit.
- Weak or missing audit trails undermine defensibility during OIG investigations and payer reviews, turning routine inquiries into costly remediation efforts.
- PHI exposure through incomplete BAAs triggers HIPAA liability even without an actual data breach.
- Unmonitored vendor obligations mean organizations cannot verify whether third parties are meeting the performance, security, or reporting standards their contracts require.
- Untracked billing and reimbursement terms lead to underpayments, denied claims, and revenue leakage that compounds over time.
These risks rarely exist in isolation, and managing them manually only makes the problem harder to contain.
How technology improves contract compliance in healthcare
Manual contract management cannot keep pace with healthcare's regulatory complexity. When agreements are scattered, compliance becomes reactive. Teams discover problems after a deadline has passed, an audit has been initiated, or a vendor has fallen out of compliance.
Healthcare contract management platforms shift this dynamic by centralizing documents, automating deadline tracking, and creating the audit trails that regulators expect.
Here’s what changes with the right platform:
- Standardized templates keep regulatory language consistent across departments, reducing clause-level compliance gaps.
- Role-based access controls restrict who can view or modify contracts containing PHI.
- Complete audit trails document every action on an agreement, from creation through execution and renewal.
- Automated contract workflows reduce time spent chasing signatures, tracking versions, and manually flagging renewals.
Technology helps a lot, but it’s not enough on its own. The real impact comes when teams pair the right tools with everyday habits that keep contracts visible, deadlines clear, and accountability shared.
Chupik Counseling, a Texas-based mental health practice with five locations, saw this shift firsthand. When they transitioned to telehealth, their paper-based consent process collapsed overnight. Patients could no longer print, sign, and return forms in person.
After evaluating other platforms and finding them overly complex for their needs, Chupik implemented Signeasy's templates for patient consent forms and HIPAA-compliant telemedicine agreements.
The result: automated consent collection via email, immediate digital filing for therapists, and 50 to 100 tele-consents processed per week.
Read the full case study
Tips for managing contract compliance in healthcare
Technology helps, but it works best when paired with the right operational habits. These seven practices address the areas where compliance gaps are most likely to form: contract visibility, deadline management, and accountability across teams.
1. Centralize all contracts in a single repository
When payer agreements live in the finance team's shared drive, BAAs sit in legal's inbox, and vendor contracts are filed locally on a department head's laptop, no one has a complete picture of the organization's compliance posture. A contract compliance audit request for "all active vendor agreements with PHI access" becomes a multi-day exercise in tracking down files across departments.

A centralized repository eliminates this problem. Every agreement, regardless of department or contract type, is stored in one searchable location with consistent metadata: status, counterparty, renewal date, and key obligations.
Signeasy's Intelligent Contract Management uses AI to auto-tag key terms and extract metadata on upload. Contracts are organized into Spaces with role-based access, and Smart Search lets teams locate agreements by clause, obligation, or renewal date in seconds.
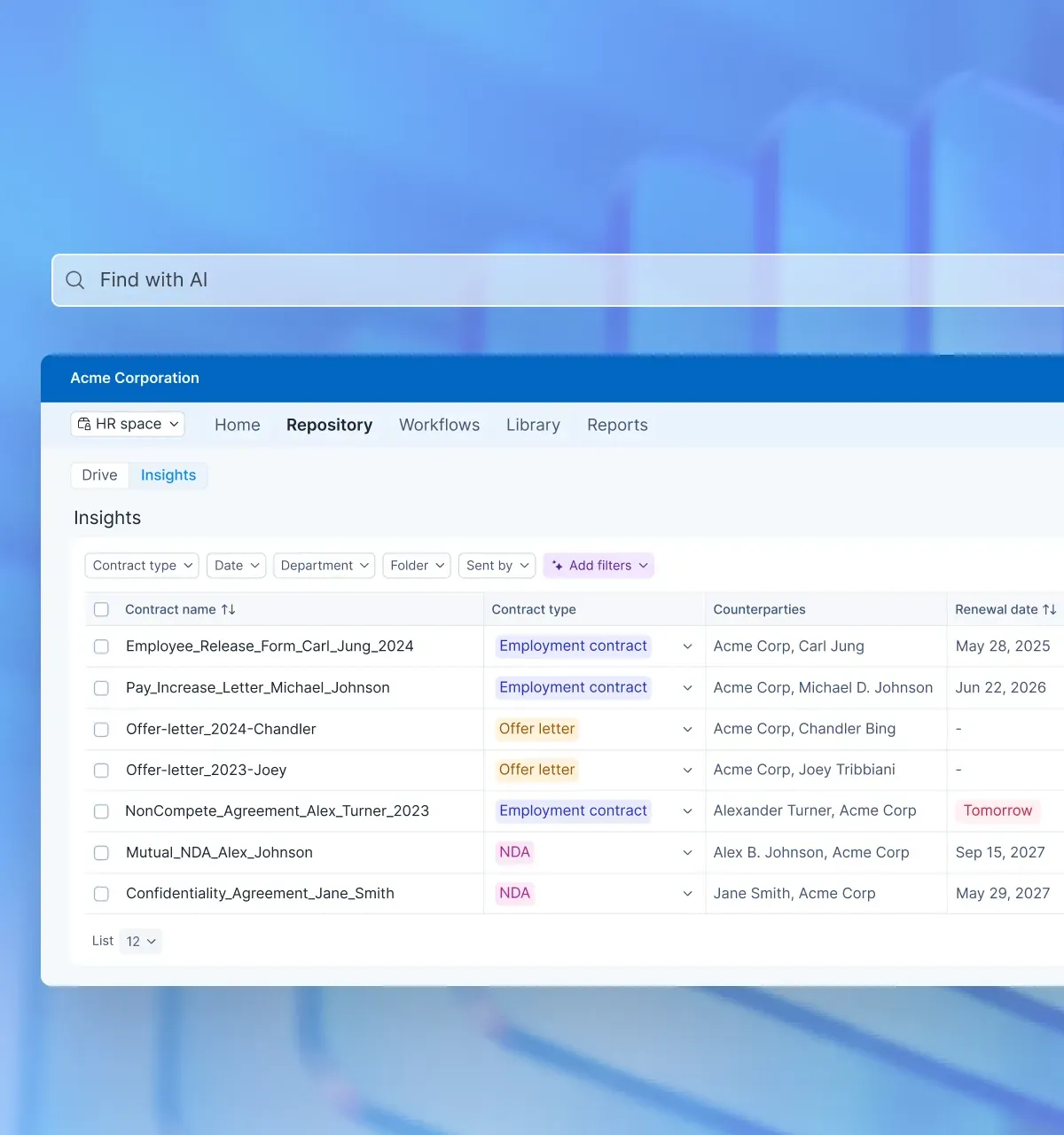
2. Automate renewal alerts and compliance deadlines
A lapsed BAA does not send a notification, nor does a payer contract that auto-renewed on last year's reimbursement rates. These failures stay invisible until they surface as financial losses or regulatory findings.
Automated alerts tied to contract milestones ensure the right stakeholders are notified before deadlines pass. The key is putting these reminders where teams already work.
Signeasy integrates renewal and milestone reminders directly with Google, Apple, and Outlook calendars. Stakeholders receive alerts ahead of expiration dates, obligation deadlines, and compliance checkpoints without relying on manual tracking.

Suggested read: Contract Compliance Reporting: A Practical Guide
3. Standardize contract templates and pre-approved clauses
Every time a department drafts a BAA or vendor agreement from scratch, there is a risk that required HIPAA clauses get omitted, liability language gets altered, or termination terms shift without legal review.
Across dozens of departments and hundreds of contracts, this creates systemic compliance exposure.
A template library with pre-approved regulatory language eliminates this at the source. Teams select the right template, customize variable fields (vendor name, scope, pricing), and send for signatures. The compliance language stays locked.
Signeasy's contract templates let administrators build compliant starting points for patient consent forms, BAAs, vendor agreements, and service contracts. Guided signing fields reduce errors and omissions, and teams can reuse templates across departments without risk of altering protected clauses.
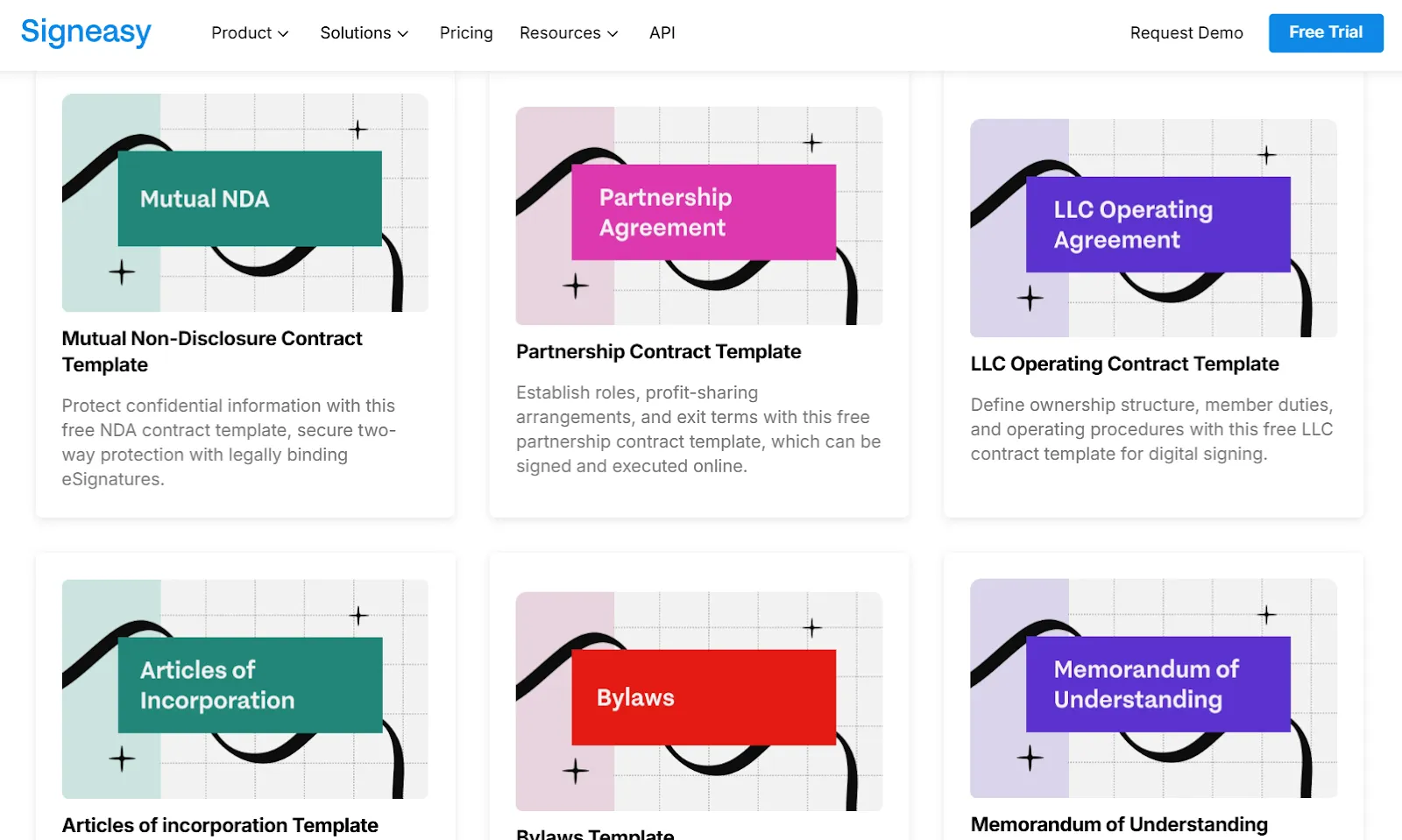
4. Enforce role-based access controls
In healthcare, role-based access is a HIPAA requirement for any system that handles protected health information.
What’s more, a billing coordinator and a chief medical officer should not have the same level of contract access. Without proper controls, physician compensation agreements, payer rate schedules, and PHI-containing BAAs are exposed to unauthorized viewing or editing.
Signeasy supports role-based permissions within dedicated Spaces, along with two-factor authentication (2FA), SSO, and tamper-proof Trust Seals on every signed document. Administrators control who can send, sign, or view contracts at the team level.
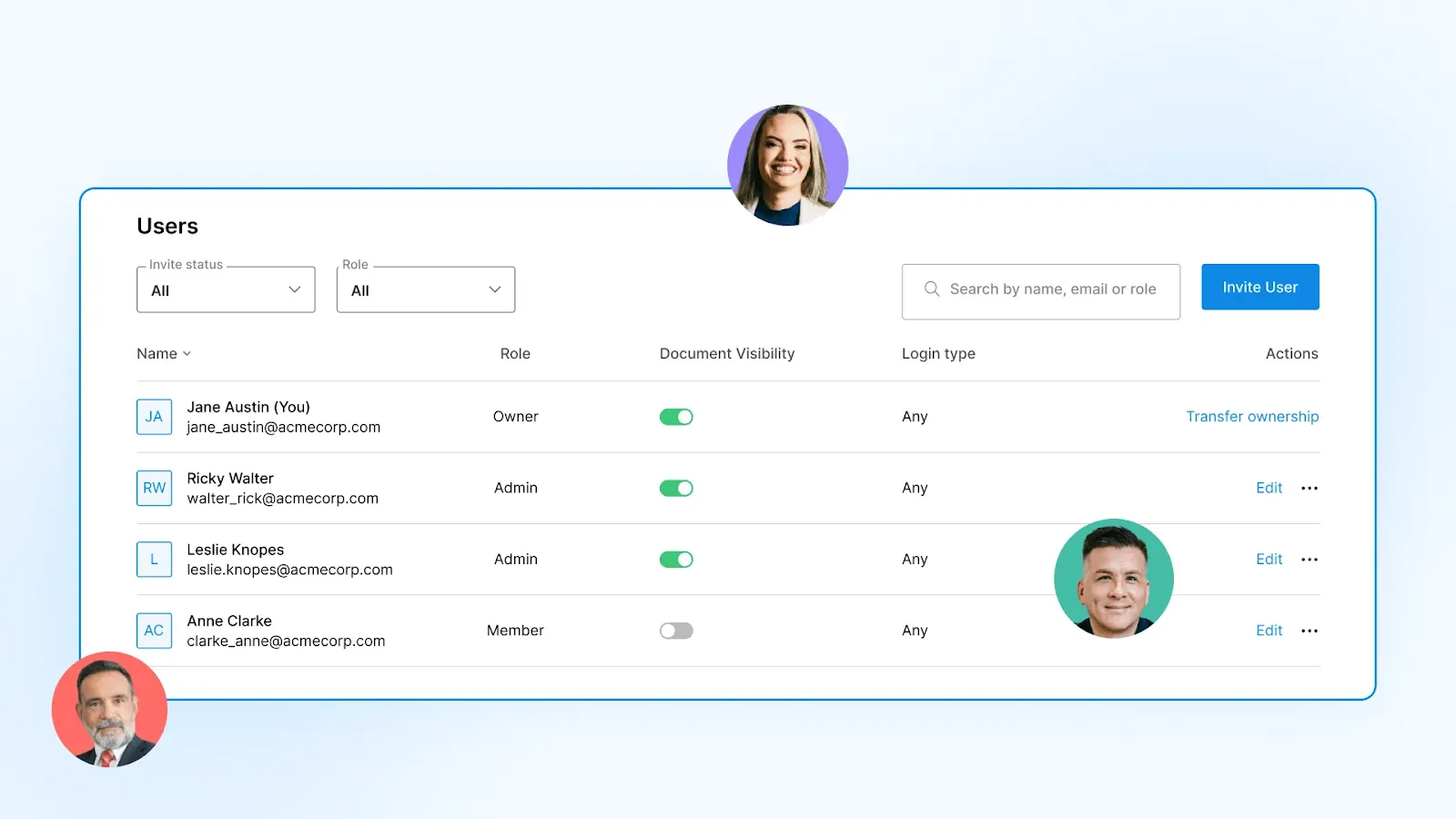
5. Conduct regular contract audits
Routine contract compliance audits surface the problems that daily operations miss: billing terms that no longer match reimbursement patterns, vendor obligations that were never fulfilled, BAAs that have not been updated since the last regulatory change, and amendments made without proper documentation.
Here are some key questions to raise during your audits:
- Are all parties meeting their contractual obligations?
- Do billing terms match actual reimbursement patterns?
- Are BAAs and vendor agreements aligned with current HIPAA requirements?
- Have any amendments been made without documentation or approval?
Pro Tip: We recommend quarterly reviews for high-risk contracts (payer agreements, BAAs), and annual reviews for lower-risk vendor and service agreements. It’s also helpful to conduct an audit after any major regulatory update.
6. Build cross-departmental collaboration into contract workflows
A single vendor agreement can require input from legal, finance, clinical leadership, and operations before it is ready for execution. When these teams work in silos, approvals stall, version control breaks down, and no one has visibility into where the contract stands.

Sequential signing and approval workflows route contracts through each stakeholder in the correct order, with clear visibility into who has reviewed, who is pending, and where delays are occurring.
Signeasy's collaboration tools support multi-party review with sequential and parallel signing, real-time status tracking, and automatic notifications at every approval stage.
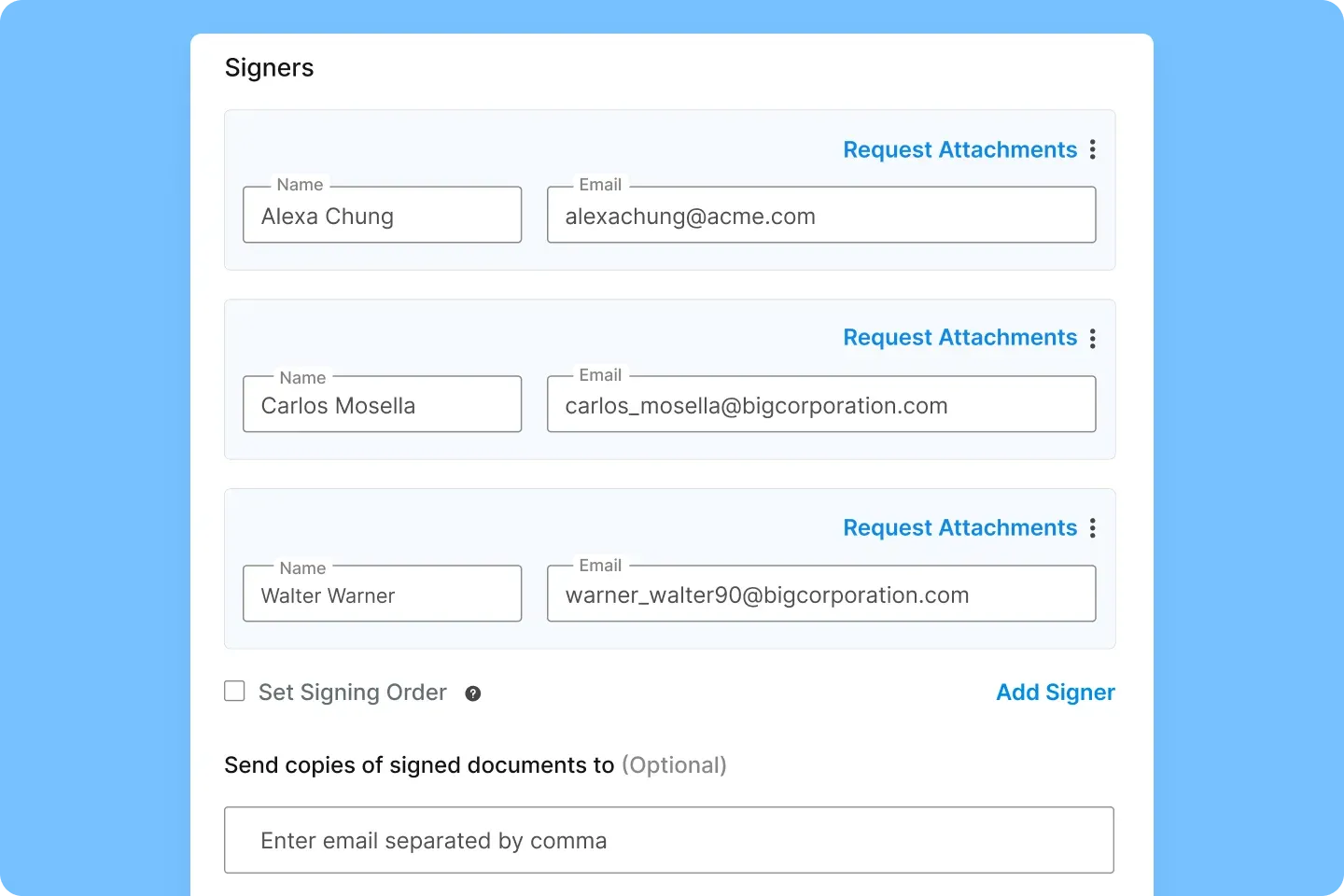
7. Invest in staff training on compliance processes and tools
Training gaps are among the most common findings in healthcare compliance audits.
Staff need to understand three things:
- How to use the contract management tools
- How HIPAA obligations apply to contract handling
- How internal workflows for routing, reviewing, and escalating contracts work
Platforms (like Signeasy) are designed for ease of adoption to reduce this burden.
When staff can sign from mobile devices, search contracts in natural language, and receive automated reminders without navigating a complex enterprise system, compliance becomes part of daily workflow rather than a separate task to manage.
How Signeasy supports contract compliance in healthcare
The tips above work best when paired with a platform built for the demands of healthcare contract workflows. Signeasy is a contract management platform that brings HIPAA-compliant eSignature, automation, storage, and compliance capabilities together in one place.
Here’s how Signeasy helps healthcare teams stay compliant across the contract lifecycle.
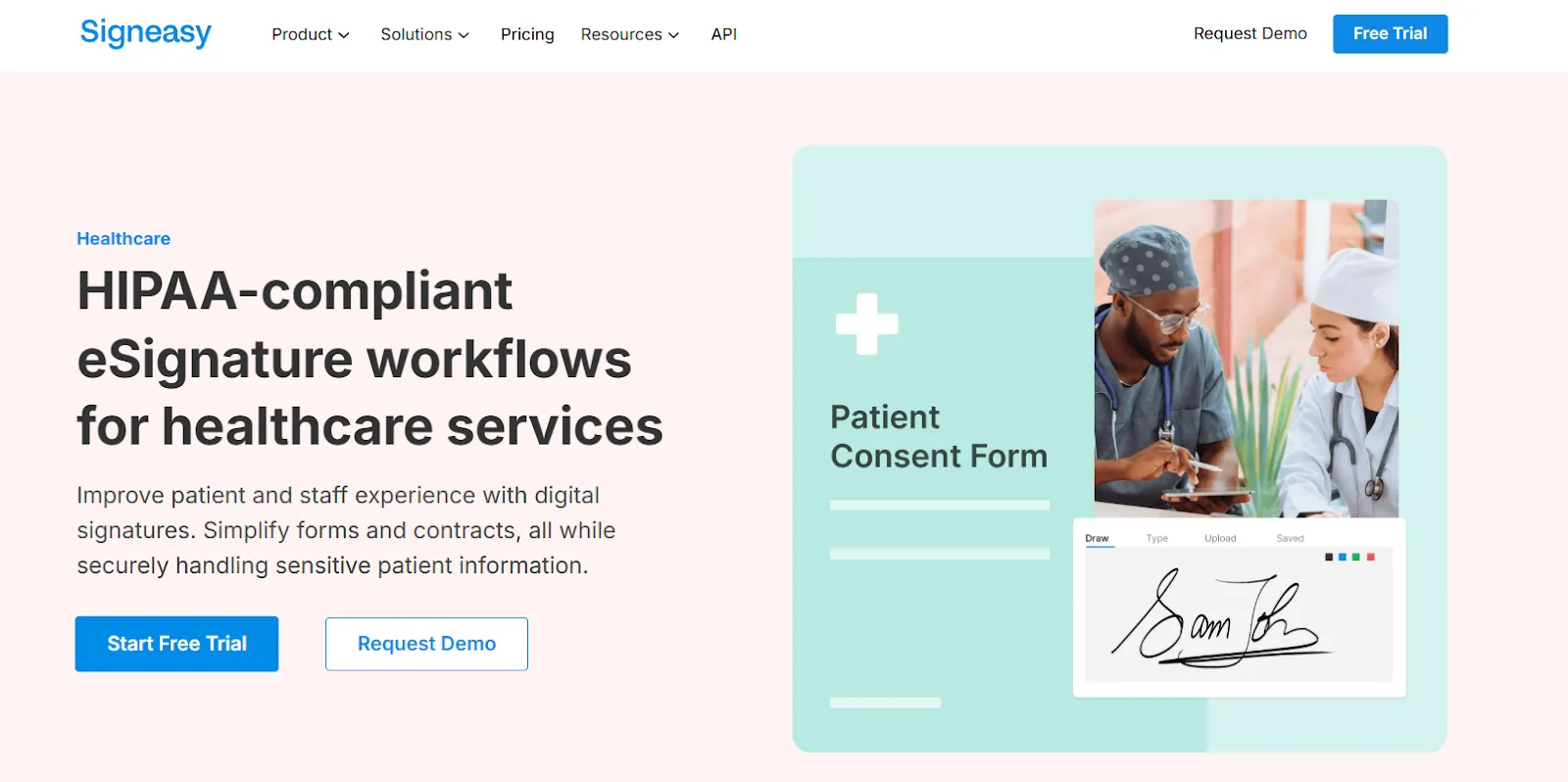
1. Stay audit-ready with HIPAA-compliant eSignature workflows
Every document signed using Signeasy’s electronic signatures for healthcare contracts includes a detailed audit trail that logs signer identity, timestamps, IP addresses, email addresses, and device data.
These records support HIPAA accountability requirements and provide clear documentation during internal reviews or external audits. Signeasy also supports compliance with SOC 2, ESIGN, UETA, and eIDAS standards.
2. Meet FDA requirements with 21 CFR Part 11 support
For organizations operating in FDA-regulated environments, Signeasy's Build Your Plan for enterprises supports 21 CFR Part 11 compliance. Healthcare institutions and life sciences companies handling clinical documentation and electronic records can meet federal validation requirements without adding separate tools to their workflow.

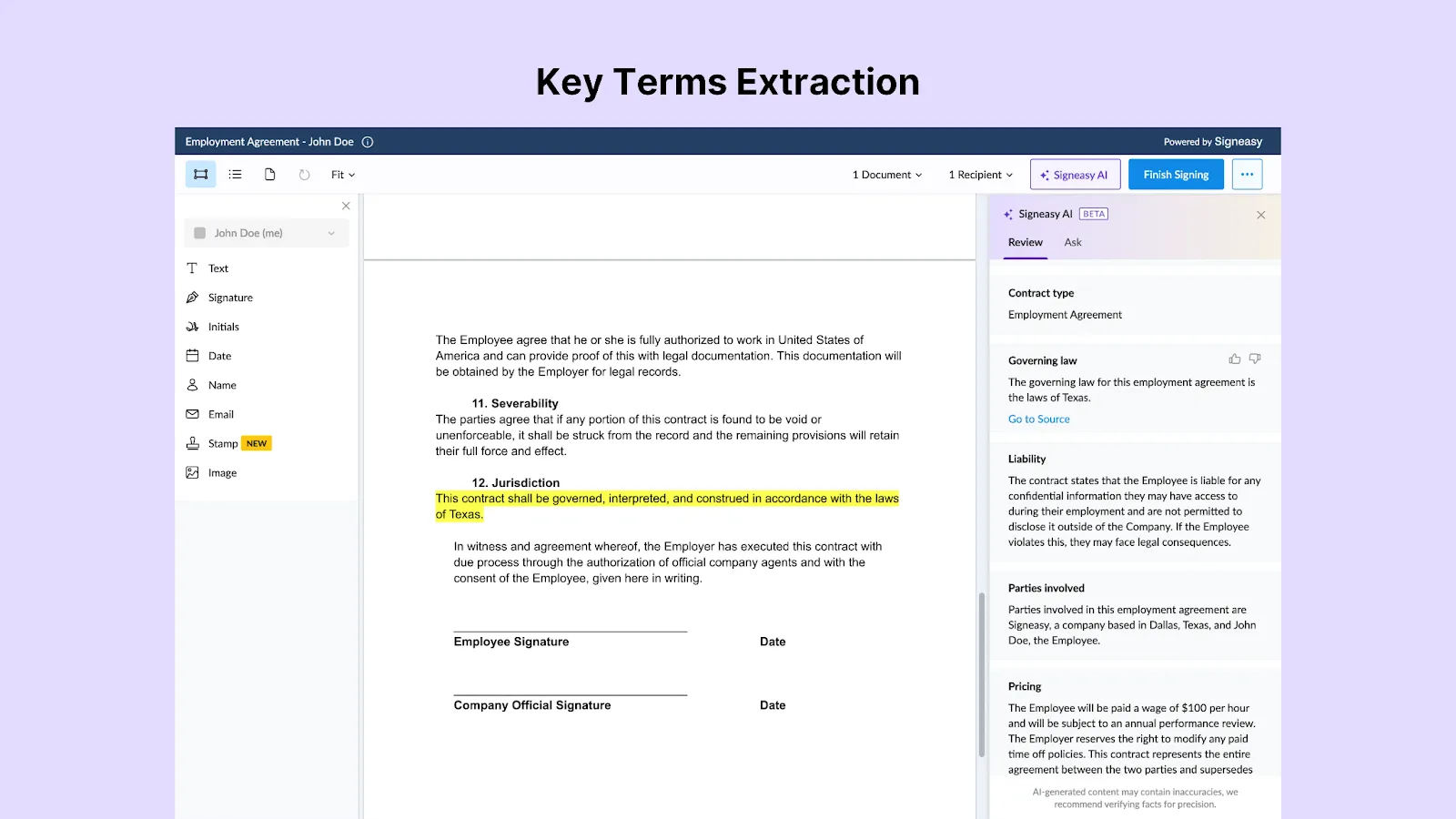
3. Review contracts quickly with AI-powered summaries and key terms
Within each document, Signeasy's AI generates concise contract summaries and extracts key terms such as payment conditions, renewal dates, and termination clauses. Healthcare teams can use Smart Q&A to ask natural language questions about a contract and receive instant answers sourced directly from the document.
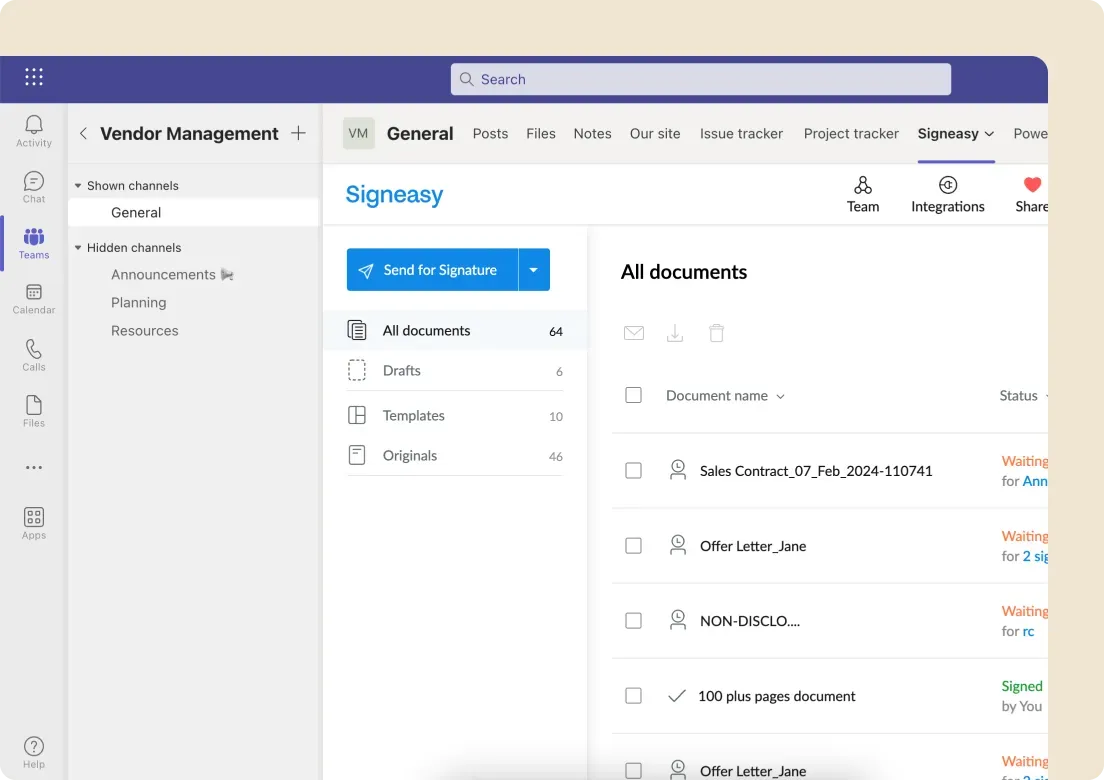
4. Keep contracts flowing inside the tools your team already uses
Signeasy connects with the platforms that healthcare organizations already rely on. Teams can make efficient contract workflows through Signeasy’s integrations, like Microsoft SharePoint for structured document management, Outlook to send and track contracts without leaving their communication tools, and HubSpot to automate agreements using CRM data.
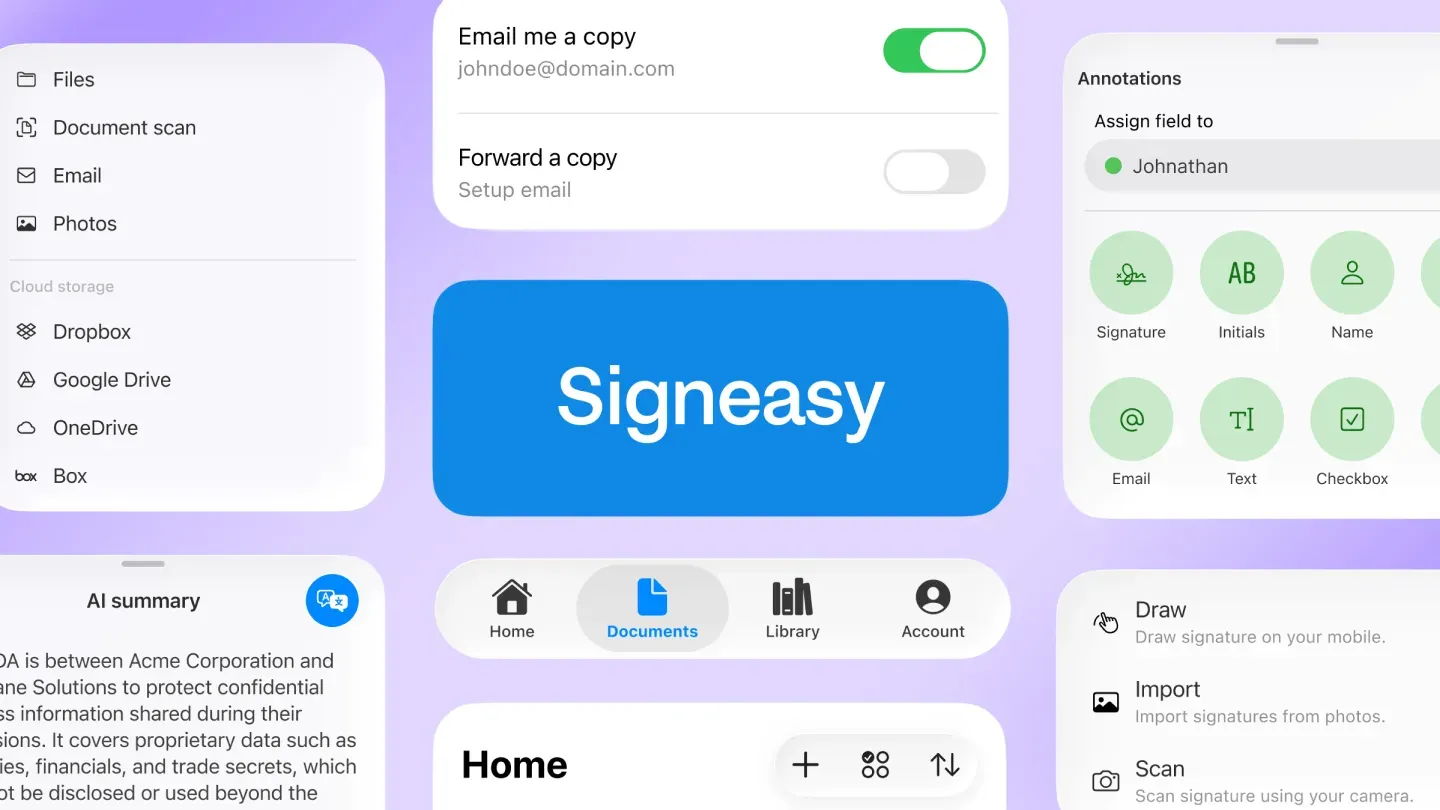
5. Collect signatures at the point of care with iPad and mobile apps
Healthcare staff can collect signatures at the point of care using Signeasy's iOS, Android, and iPad apps.
In-person signing on tablets is particularly useful in clinical settings, patient intake areas, and field operations. As a secure eSignature solution, it removes the storage and backup risks that come with printed paperwork, while keeping admissions and vendor check-ins moving.
6. Embed eSignature workflows into internal healthcare systems
Signeasy's eSignature API lets development teams embed document signing directly into patient portals, EHR systems, or custom onboarding applications.
Staff no longer need to toggle between platforms, and contract workflows stay within the existing infrastructure.
Build a compliance-first contract culture in healthcare
Healthcare contract compliance demands consistent oversight, clear processes, and tools that match the complexity of the industry.
The tips in this guide, from centralizing contracts to automating alerts and enforcing access controls, offer a practical path to reducing risk across departments. Applied consistently, they help close the gaps that hurt healthcare organizations most: contracts renewing on unfavorable terms, billing mismatches draining revenue, and outdated clauses creating audit exposure.
Signeasy brings these practices together in one contract management platform. Healthcare teams get HIPAA-compliant eSignature workflows, AI-powered contract insights, and integrations with Microsoft SharePoint, Teams, and Google Workspace.
Development teams can also use the API to embed signing directly into internal systems. The result is stronger compliance without added operational friction.
Start free trial to build compliant contract workflows with Signeasy from day one.










.png)
.png)
.png)